Prevention of Cervical Cancer in Sub-Saharan Africa: The Advantages and Challenges of HPV Vaccination
University of New South Wales
"[H]igh vaccine coverage and sustainable programs can be delivered with strong commitment from government, comprehensive planning with ministries of health as well as education, and early community sensitisation."
This article describes epidemiological features of cervical cancer in sub-Saharan Africa (SSA) and the current status of human papillomavirus (HPV) vaccine implementation in SSA countries. Rwanda's experience of achieving high vaccination coverage in their national HPV immunisation programme is used as a case study to examine factors such as government ownership and support, school-based delivery, social mobilisation, and strategies for reaching out-of-school girls. These findings might be applied to other SSA countries planning for HPV vaccination.
The article begins by describing the significant burden from cervical cancer in SSA and the role for HPV vaccination. In short, while alternative screening types suitable for low- and middle-income countries (LMICs) now exist, challenges to implementation have meant they are still not widely available, and uptake of screening remains low. Primary prevention of cervical cancer with HPV vaccination is thus particularly important in SSA. As of June 2018, there were 8 countries in SSA with a national HPV immunisation programme, and nearly twice as many with pilot programmes. Rwanda achieved extremely high vaccine coverage of greater than 98% for the 3-dose schedule of vaccinations in 2014.
As reported here, Rwanda's national HPV vaccination programme was planned with extensive input from a variety of stakeholders, including the Ministry of Education (MOE) and health workers. Planning involved, among other things, information dissemination strategies. A nationwide sensitisation campaign was rolled out before vaccinations began. Community partnerships were established, with inclusion of local leaders, community health workers, and teachers. Information was provided by health workers, government, and the media; in addition, teachers and health workers informed students about the vaccine. Schools were used as the delivery platform, which was effective, as school attendance in Rwanda is greater than 98%. Community health workers identified and vaccinated girls not attending school, through registration records from health centres.
An ecological study of 45 LMICs with HPV demonstration projects or national programmes cited in the article showed that countries that had achieved high coverage had employed good social mobilisation and community engagement strategies. This reinforces the Rwandan experience, as dissemination of knowledge is critical to successful implementation of vaccination programmes. A cross-sectional study of adolescents and health workers from Uganda found that vaccine uptake in the study population was only 14%, and both health workers and adolescents had limited awareness of the importance of the vaccination.
The article concludes by outlining factors that have facilitated some countries, such as Rwanda, to overcome challenges such as lack of awareness and to achieve high HPV vaccine coverage.
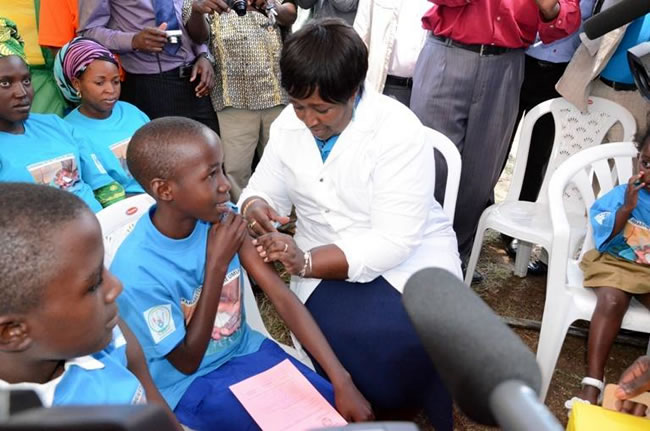
Vaccines (Basel) 6(3): 61. doi: 10.3390/vaccines6030061. Image credit: World Health Organization (WHO) Regional Office for Africa
- Log in to post comments












































