Community Acceptability of Use of Rapid Diagnostic Tests for Malaria by Community Health Workers in Uganda
Makerere University School of Public Health (Mukanga, Kallander); Karolinska Institutet (Mukanga, Waiswa, Kallander); African Field Epidemiology Network (Mukanga, Ojiambo); Malaria Consortium Africa (Tibenderana, Mutamba, Counihan, Kallander); Makerere University (Kiguli, Pariyo, Waisw); Mbarara University of Science and Technology (Bajunirwe).
Published in the Malaria Journal, this article shares findings of a study to assesses community acceptability of the use of rapid diagnostic tests (RDTs) by Ugandan community health workers (CHWs), locally referred to as community medicine distributors (CMDs). According to the article, many malaria endemic countries plan to introduce artemisinin combination therapy (ACT) at community level using CHWs for treatment of uncomplicated malaria, but use of ACT with reliance on presumptive diagnosis may lead to excessive use, increased costs, and rise of drug resistance. Use of rapid diagnostic tests (RDTs) could address these challenges but only if the communities will accept their use by CHWs. The article suggests that a well-designed behaviour change communication strategy is needed to address the anticipated programmatic challenges as well as community fears and stigma about drawing blood.
The study was conducted in Iganga district in Uganda using 10 focus group discussions (FGDs) with CMDs and caregivers of children under five years, and 10 key informant interviews (KIIs) with health workers and community leaders. Pre-designed FGD and KII guides were used to collect data. Manifest content analysis was used to explore issues of trust and confidence in CMDs, stigma associated with drawing blood from children, community willingness for CMDs to use RDTs, and challenges anticipated to be faced by the CMDs.
There were four key findings of the study:
- CMDs are trusted by their communities because of their commitment to voluntarism, accessibility, and the perceived effectiveness of the anti-malarial drugs used, and their activities have led to a perception of reduced workload among health workers in health facilities;
- community members, health workers, and CMDs welcomed the use of RDTs by CMDs provided they have sufficient education level, are trained in their use, and supported to follow up children;
- fears were expressed that CMDs who collect blood using RDTs could expose the children to HIV, that the tests could be used to test children for HIV, or that the blood could be used for witchcraft; and
- CMDs were anticipated to face challenges with transport for follow up of patients and re-stocking of supplies, adults demanding to be tested, and caregivers insisting their children be treated instead of being referred.
The study found that RDTS have the potential to greatly enhance the management of febrile illness, but the success of their use by CMDs is highly dependent on how the community will accept the services provided. The acceptability of medical care by different ethnic groups is associated with the degree to which the services meet cultural values, norms, and expectations. While desirable, participatory processes in every village is not compatible with rapid national scale-up, thus a balance needs to be reached. Having CMDs of the same ethnic group, who speak the same language, and are familiar with the culture and its traditions and values are factors that can increase acceptability. The findings of this study also show that the community demand well trained CMDs to handle and interpret the tests.
Fears and stigma of taking blood of children in the community were common in the study groups, relating both to risk of exposure to HIV and witchcraft. To counter for this potential threat to the programme, a well-designed behaviour change communication strategy will be required, since a successful strategy relies not only on adequately trained CMDs and the availability of drugs, but also on a well informed community. As mentioned above, this communication strategy would also address programmatic challenges, including expectations of adults to be tested and misunderstandings about the scope of work of the CHWs.
Malaria Journal on April 3 2012.
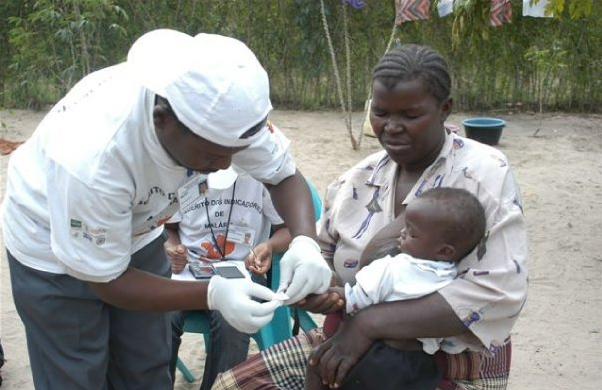
(Photo credit: Malaria Consortium)
- Log in to post comments












































